But whatever the reason, mask mandates were a fool’s errand from the start. They may have created a false sense of safety — and thus permission to resume semi-normal life. They did almost nothing to advance safety itself. The Cochrane report ought to be the final nail in this particular coffin.
There’s a final lesson. The last justification for masks is that, even if they proved to be ineffective, they seemed like a relatively low-cost, intuitively effective way of doing something against the virus in the early days of the pandemic. But “do something” is not science, and it shouldn’t have been public policy. And the people who had the courage to say as much deserved to be listened to, not treated with contempt. They may not ever get the apology they deserve, but vindication ought to be enough.
The Spectator
Browse the articles related to this topic below.
Join our community on Guilded.
Interestingly, 12 trials in the review, ten in the community and two among healthcare workers, found that wearing masks in the community probably makes little or no difference to influenza-like or Covid-19-like illness transmission. Equally, the review found that masks had no effect on laboratory-confirmed influenza or SARS-CoV-2 outcomes. Five other trials showed no difference between one type of mask over another.
https://archive.today/2023.02.03-091622/https://www.spectator.co.uk/article/do-mask-mandates-work/
Double-jabbed’ Malhotra originally supported the program, until a series of events sent him digging into the evidence. What he discovered alarmed him and resulted in the publication of two evidence-based, peer-reviewed papers along with a call for the immediate suspension of the Covid mRNA roll-out…
Over following months, emerging data led Malhotra to question whether the vaccine was linked to his father’s death. The first was an abstract published in Circulation (November 8, 2021) by US cardiothoracic surgeon, Dr Steven Gundry, who followed several hundred of his patients after the mRNA (Moderna/Pfizer) jabs. Gundry found that inflammatory markers correlated with heart disease risk went through the roof. On average, that change increased the risk of those people having a heart attack or stroke within the next five years, from 11 per cent up to 25 per cent. This increase in risk is massive.
I recall the newsroom conversations during the dark days of the pandemic only too well. They were upsetting at the time. Now, as we see a disturbing rise in excess deaths across the country, the thought of them fills me with horror and outrage.
‘You do realise these lockdowns and restrictions will end up killing people too, don’t you?’ I would say to senior editorial colleagues with something approaching desperation in my voice. ‘Sure, the virus is a serious threat to a small proportion of the population but the longer-term consequences of shutting the economy down and closing off the NHS will be deadly for huge numbers who were never at serious risk from the virus, people with years of life ahead of them. Shouldn’t we be reflecting that in our coverage? Shouldn’t we be considering the possibility that the government is going down the wrong path on this?’
The response of these colleagues would vary in tone, from patient but patronising good humour to open mockery. Many were influenced, I believe, by social media echo chambers (curated by pernicious algorithms). My colleagues had swallowed the myopic belief, adopted by people largely on the liberal left, that only lockdowns could ‘save lives’ and ‘protect the NHS’ from the devastation threatened by Covid-19. Anyone who demurred was, as far as they were concerned, clearly a right-wing lunatic.
Now we can all see how well that is working out. Provisional figures released this week reveal that more than 650,000 deaths were registered in the UK in 2022 – 9 per cent more than 2019. This is one of the largest excess death levels outside the pandemic in 50 years. But despite many of the causes of this being obvious, the BBC is pretending the development has come as something of a shock.
It isn’t mad, however, to regard the WEF as a dangerous force in global politics. The WEF is a dangerous force in global politics. To adapt Joseph Heller, just because you are paranoid, doesn’t mean the WEF isn’t after you. A shared distrust of the WEF brings together anti-capitalists on the left and culture-warriors on the right. But that distrust is based on a misunderstanding of what the WEF is these days really all about.
For many WEF critics, the vileness of the organisation can be encapsulated in one word: ‘neoliberalism.’ It’s a term that conjures up images of plutocrats and untrammelled markets ravaging the planet and exploiting blue-collar folk in the name of profit. Funnily enough, Chairman Schwab agrees with that assessment of the world’s ills. Once upon a time, the WEF prioritised the necessity and benefits of economic globalisation. That has not been the case for many years, however. In October 2020, Schwab stated that:
[S]hibboleths of our global economic system will need to be re-evaluated with an open mind. Chief among these is the neoliberal ideology. Free-market fundamentalism has eroded worker rights and economic security, triggered a deregulatory race to the bottom and ruinous tax competition.
http://archive.today/2023.01.02-193731/https://www.spectator.co.uk/article/the-davos-man-cometh/
The truth about Matt Hancock – The Spectator
Summary from The Daily Sceptic:
Mass vaccination mission creep, no rigorous vaccine safety monitoring, counter-terrorism units deployed to crush scientific and social media dissent, major restrictions pursued for political reasons without evidence, expert advisers ignored – just some of the revelations made by Isabel Oakeshott in the Spectator this week. Fresh from co-authoring Matt Hancock’s pandemic diaries, the lockdown-sceptical journalist has written down the “key lessons” she took away from the very revealing writing process she undertook with a man whose approach to the pandemic she vehemently opposes.
Wot’s in the shots? – The Spectator
So is there graphene oxide in the Pfizer shots? What Nixon found, and filmed, is bizarre to say the least. Inside a droplet of vaccine are strange mechanical structures. They seem motionless at first but when Nixon used time-lapse photography to condense 48 hours of footage into two minutes, it showed what appear to be mechanical arms assembling and disassembling glowing rectangular structures that look like circuitry and micro chips. These are not ‘manufactured products’ in the CDC’s words because they construct and deconstruct themselves but the formation of the crystals seems to be stimulated by electromagnetic radiation and stops when the slide with the vaccine is shielded by a Faraday bag. Nixon’s findings are similar to those of teams in New Zealand, Germany, Spain and South Korea.
…Nixon has shared his findings with Wendy Hoy, professor of medicine at the University of Queensland who has called on the Australian government and its health authorities to explain the apparent spontaneous formation of chips and circuitry in mRNA vaccines when left at room temperature, and the abnormal objects that can be seen in the blood of vaccinated people. Hoy thinks that these are ‘undoubtedly contributing to poor oxygen delivery to tissues and clotting events, including heart attacks and strokes’ and asks why there is no systematic autopsy investigation of deaths to investigate the role of the vaccine in Australia’s dramatic rise in mortality.
http://archive.today/2022.11.06-144656/https://www.spectator.com.au/2022/11/wots-in-the-shots/
Are masks bad for you? – The Spectator
Could masks be making us sick? That’s the suggestion in a Japanese study, published this week in Nature’s Scientific Report’s journal, which looked at bacterial and fungal growth on face masks worn during the pandemic. The results may put you off your tea.
The study looked at the masks of 109 people and shows that bacteria grows in bigger colonies on the inside of the mask compared with the outside. The opposite was true for fungus. Wearing the same mask for a long period of time ‘significantly’ increased the amount of fungus growing on a mask but had no effect on the amount of bacteria.
Every mask bar one – 99 per cent of the masks examined – contained bacterial colonies on the inside and 94 per cent on the outside. The type of mask worn – cloth or disposable – made no difference to the spread of bacteria. On the other hand, fungus was found on the outside of 95 per cent of masks and on the inside of 79 per cent. An interesting finding was that bacterial counts were lower on the insides of masks worn by women. It suggested this may be because they wear makeup and take better care of their skin.
http://archive.today/2022.12.10-112124/https://www.spectator.co.uk/article/are-masks-bad-for-you/
The NHS has started warning people to take extra precautions, a degree of fear and concern is undeniably being created. Yet, monkeypox seems to be a not especially contagious viral infection that isn’t particularly dangerous.
Something that became all too apparent during the Covid panic was the failure of either the general population or most of the media to put things in context. We’re seeing the same again with the monkeypox scare. The Spectator published this table on May 23rd showing that in this recent scare there have been to date 56 cases of monkeypox in England and 170 worldwide.
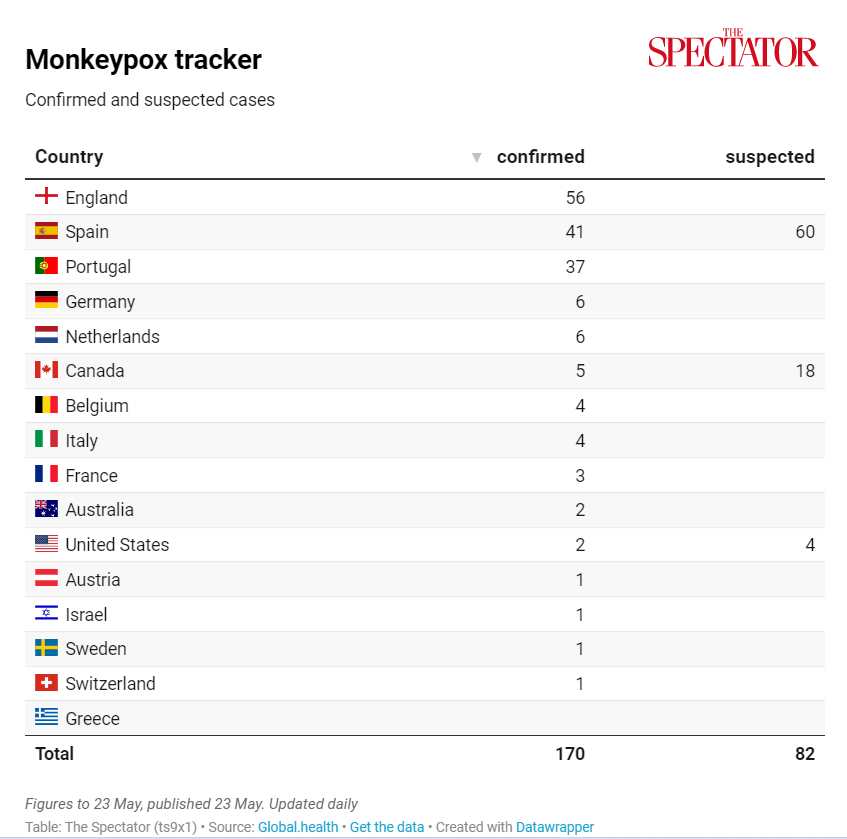
https://dailysceptic.org/2022/05/24/whats-so-special-about-monkeypox/
Google once believed it could use algorithms to track pandemics. People with flu would search for flu-related information, it reasoned, giving the tech giant instant knowledge of the disease’s prevalence. Google Flu Trends (GFT) would merge this information with flu tracking data to create algorithms that could predict the disease’s trajectory weeks before governments’ own estimates.
But after running the project for seven years, Google quietly abandoned it in 2015. It had failed spectacularly. In 2013, for instance, it miscalculated the peak of the flu season by 140 per cent.
According to the German psychologist Gerd Gigerenzer, this is a good example of the limitations of using algorithms to surveil and study society. The 74-year-old has just written a book on the subject, How to Stay Smart in a Smart World. He thinks humans need to remain in charge in a world increasingly filled with artificial intelligence that tries to replicate human thinking.
It is more than a rebuke to Medley and the modellers though. This pandemic began, for many, with an announcement from Imperial College, whose study predicted 500,000 deaths if we did nothing. We locked down and never tested the prediction.
This time, in the face of what the public saw as dire predictions, we didn’t lock down and the apocalypse never came. The unspoken — and sometimes spoken — implication is clear: are we all fools?
The consequences of this unprecedented state-sanctioned campaign have been visible everywhere: from the old lady in the street, paralysed with fear of contamination from another human, darting into the road to avoid someone walking the other way, to the neighbour donning a face covering and plastic gloves to wheel the dustbin to the end of her drive. These kinds of incidents are the product of an intensive messaging campaign, designed by the government’s behavioural scientists, to ‘nudge’ us into compliance with the Covid-19 restrictions and the subsequent vaccine rollout.
The analysis identified 72 studies that might potentially have provided evidence on the effectiveness of masks, social distancing and hand washing. Of those, just six (not eight, 30 or 72) were sufficiently relevant — and of sufficient quality — that they could provide any useful information on mask efficacy. And how reliable were the six? Four were assessed to have a moderate risk of bias, and two to have a serious or critical risk.
Four months ago, I had my second dose of the Pfizer Covid-19 vaccine. I work for the NHS and fully support Britain’s vaccination campaign, so it was a simple decision for me to make. I had no problems with my first dose and I knew that the vaccines have been found to be highly effective and safe, preventing up to 96 per cent of Covid hospitalisations.
The day after my second dose I began to feel some aches and pains, but I gave little thought to the vaccine and carried on as normal. Four days later though my chest was seriously aching. I tried various stretches and painkillers but my symptoms grew worse. Then there was a sharp pain, piercing into the left side of my chest, near my heart. After a quick call to NHS 111, they sent me directly to Accident & Emergency, where I was strapped up to an electrocardiogram (ECG) machine and given blood tests to see if I was having a heart attack. I’m in my early thirties and relatively healthy, with no family history of heart disease or underlying conditions, and I’d never felt this sensation before.
In August, Public Health England released data which shows that vaccination does not appreciably guard against Covid infection and transmission and protection worked out at around 17 per cent for the over-fifties. As I observed then, this would mean the vaxxed and unvaxxed pose a comparable danger to each other. All Covid apartheid schemes are therefore insensible.
Fresher information has fortified this conclusion of the summer. In every age group over 30 in the UK, the rates of Covid infection per 100,000 are now higher among the vaxxed than the unvaxxed. Indeed, in the cohorts aged between 40 and 79, infection rates among the vaccinated are more than twice as high as among the unvaccinated. PHE’s fruitlessly rechristened body, the UK Health Security Agency, frantically clarifies that the data ‘should not be used to estimate vaccine effectiveness’, a caveat which I include for the sake of accuracy. But the differences in the infection rates are drastic enough for you to draw your own conclusions.
Our government has used Covid as an excuse to turn Australians into digital products. It is the perfect scam. Every dictatorship knows that humans are cheap, renewable, and disposable. Our digital identities are worth a fortune to the right third-party buyer, while the ability to track and control our movements presents a unique opportunity for politicians wishing to manage democracy instead of being a victim of its whims.
So what about Sweden, huh? – The Spectator
It’s amazing how often Sweden still crops up in conversations. It didn’t impose tough lockdown, kept primary schools and core economic activities functioning, issued clear guidelines and relied on voluntary social distancing and personal hygiene practices to manage the crisis. For harsh lockdowns to be justified elsewhere, Sweden had to be discredited. Hence the harsh criticisms of Sweden’s approach last year by the New York Times, Newsweek, USA Today, CBS News and others.
But with Sweden’s demonstrable success, goalposts have shifted. Every time it’s mentioned as a counter to Europe’s high Covid-toll lockdown countries, the response now is: ‘But their Nordic neighbours did much better. Look at Denmark’. Let’s ‘interrogate’ this argument.
I had no choice but to speak out against lockdowns. As a public-health scientist with decades of experience working on infectious-disease outbreaks, I couldn’t stay silent. Not when basic principles of public health are thrown out of the window. Not when the working class is thrown under the bus. Not when lockdown opponents were thrown to the wolves. There was never a scientific consensus for lockdowns. That balloon had to be popped.
…Ultimately, lockdowns protected young low-risk professionals working from home – journalists, lawyers, scientists, and bankers – on the backs of children, the working class and the poor.
https://www.spiked-online.com/2021/06/04/why-i-spoke-out-against-lockdowns/
So, the third wave is officially no more. New modelling by SPI-M, the government’s committee on modelling for pandemics, has, at a stroke, eradicated the predicted surge in new infections, hospital admissions and deaths which it had pencilled in for the autumn or winter as a result of lockdown being eased.
…As Philip Thomas explained here on Sunday, Imperial College has also assumed strangely low estimates for the number of people in Britain carrying antibodies. If you are going to use assumptions that are far more pessimistic than real world data suggests, it is small wonder that SPI-M keeps predicting waves and surges that turn out to be wide of the mark. The question is: why are these modelling teams using such negative assumptions?
https://www.spectator.co.uk/article/how-likely-is-a-third-wave-
The retired Justice of the Supreme Court admits breaking lockdown regulations and seems willing to countenance civil disobedience
…So most readers will turn first to Sumption’s final chapter, about the Covid pandemic. His target is not just the government and its decision to exercise ‘coercive powers over its citizens on a scale never previously attempted [and] with minimal parliamentary involvement’. He also blames the public for voluntarily surrendering their liberty ‘out of fear of some external threat’ — and MPs for agreeing to work remotely. Because this chapter was written as a lecture in October, it makes no mention of the government’s successful vaccination programme. His prediction that ‘Britain seems likely to suffer greater economic damage than almost every other European country’ is one he might now reconsider.
https://www.spectator.co.uk/article/despotic-laws-can-even-should-be-ignored-says-jonathan-sumption