Presented as an independent voice for “unbiased” scientific advice, iSAGE provided a channel for media spinmeisters, spies and psy-op specialists to influence Britain’s pandemic policy without accountability. Leaked internal emails show members fretting over its unethical methods.
Public Health England
Browse the articles related to this topic below.
Join our community on Guilded.
UK health and statistics authorities allegedly used 14 inconsistent ways to define fatalities.
Many who died early in the pandemic were never actually tested for the virus while others may have died from something else entirely, according to experts.
…The Oxford study, from 800 freedom of information requests, found some deaths were attributed to Covid just because a care home provider said so and coronavirus was rife.
The report stated: “At the beginning of the pandemic, Public Health England linked data on positive cases to the NHS central register of patients who died.
“This definition meant that a patient who tested positive would be counted as a Covid death even if they were run over by a bus several months later.”
It has been one of the most enduring Covid conspiracy theories: that the ‘gold standard’ PCR tests used to diagnose the virus were picking up people who weren’t actually infected.
Some even suggested the swabs, which have been carried out more than 200 million times in the UK alone, may mistake common colds and flu for corona.
If either, or both, were true, it would mean many of these cases should never have been counted in the daily tally – that the ominous and all-too-familiar figure, which was used to inform decisions on lockdowns and other pandemic measures, was an over-count.
And many of those who were ‘pinged’ and forced to isolate as a contact of someone who tested positive – causing a huge strain on the economy – did so unnecessarily.
Such statements, it must be said, have been roundly dismissed by top experts. And those scientists willing to give credence such concerns have been shouted down on social media, accused of being ‘Covid-deniers’, and even sidelined by colleagues.
But could they have been right all along?
Scientists did not have accurate Covid case numbers, and were unsure of hospitalisation and death rates when they published models suggesting that more than 500,000 people could die if Britain took no action in the first wave of the pandemic, it has emerged.
On March 16 2020, Imperial College published its “Report 9” paper suggesting that failing to take action could overwhelm the NHS within weeks and result in hundreds of thousands of deaths.
Before the paper, the UK coronavirus strategy was to flatten the peak rather than suppress the wave, but after the modelling was made public, the Government made a rapid u-turn, which eventually led to lockdown on March 23.
However SPI-M (Scientific Pandemic Influenza Group on Modelling) minutes released to the Telegraph under a Freedom of Information request show that by March 16, modellers were still “uncertain” of case numbers “due to data limitations”.
The minutes show that members were waiting for comprehensive mortality data from Public Health England (PHE) and said that current best estimates for the infection fatality rate, hospitalisation rates, and the number of people needing intensive care were still uncertain.
They also believed that modelling only showed “proof of concept” that lockdowns could help, and warned that “further work would be required”.
Published September 2018
The behavioural and social sciences are the future of public health. Evidence from behavioural science suggests that simple and easy ways of helping people to change their behaviour are the most effective. Whether it’s encouraging smokers to quit, increasing uptake of the NHS Health Check, making healthier food choices easier, or reducing the number of inappropriate antibiotic prescriptions, this evidence can help in understanding and therefore influencing behaviour change that promotes health, prevents disease, and reduces health inequalities. We must reach and be meaningful to people in the lives that they are leading.
It is time for the public health system to advance the use of behavioural and social sciences, and for this purpose, PHE’s Behavioural Insights experts, working with many partners, have led the collaborative development of this comprehensive strategy – the first of its kind in the field.
For commentary on this document, see UK Column News, 23rd February 2022.
For months the British public have been deceived with tales that there are just 5 million people in the United Kingdom who have refused to take up the offer of a Covid-19 vaccine. But today we can reveal that this is a lie.
It is a complete fabrication that has no doubt been used to make those who have refused the jab feel as if they are part of a minority, because an official UK Government report proves that in England alone there are approximately 23.5 million people who have not had a single dose of a Covid-19 vaccine.
In August, Public Health England released data which shows that vaccination does not appreciably guard against Covid infection and transmission and protection worked out at around 17 per cent for the over-fifties. As I observed then, this would mean the vaxxed and unvaxxed pose a comparable danger to each other. All Covid apartheid schemes are therefore insensible.
Fresher information has fortified this conclusion of the summer. In every age group over 30 in the UK, the rates of Covid infection per 100,000 are now higher among the vaxxed than the unvaxxed. Indeed, in the cohorts aged between 40 and 79, infection rates among the vaccinated are more than twice as high as among the unvaccinated. PHE’s fruitlessly rechristened body, the UK Health Security Agency, frantically clarifies that the data ‘should not be used to estimate vaccine effectiveness’, a caveat which I include for the sake of accuracy. But the differences in the infection rates are drastic enough for you to draw your own conclusions.
Only six healthy children with no underlying health conditions died as a direct result of catching Covid during a 12-month window, NHS analysis has revealed.
Four died from Covid, while two developed a Kawasaki-like inflammatory condition called Pims-TS, caused by the virus.
The data calls into question the wisdom of closing schools and forcing children to spend months at home when the health risk to under-18s is so small.
Children ‘have 99.995 per cent chance’ of surviving virus
Each line in the above table describes “vaccine effectiveness”. That is how much the vaccine REDUCES chances of illness compared to the unvaccinated. The red numbers are NEGATIVE, meaning that vaccine INCREASES chances of geting Covid, compared to the unvaccinated. For example, for vaccinated 40-49 year olds, their chances of getting covid are (see above) 2.28 TIMES HIGHER than the unvaccinated. So their vaccine is a Covid magnet. No kidding.
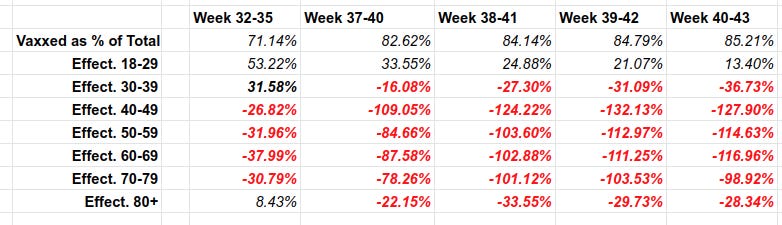
Over 82% of deaths in the UK are among the vaccinated.
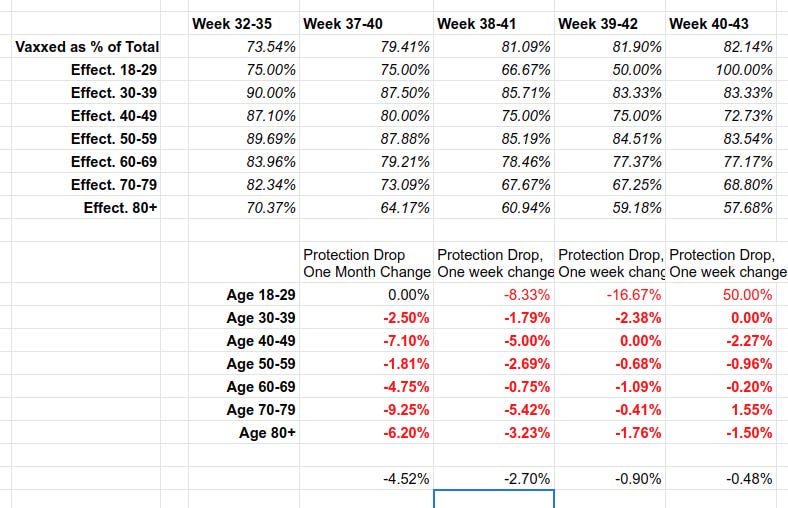
https://igorchudov.substack.com/p/uk-vaccines-weekly-ineffectiveness
To give you a preview of this article: Vaccines in the UK have become LESS THAN WORTHLESS in October. “The vaccinated” get infected MORE than the unvaccinated. The vaccinated have higher infection rates and are now the drivers of the UK epidemic. While some degree of “protection from death” still remains, it is dropping by about 7% every month for the most relevant groups. I break it down by age to avoid the stupid “but you need to do age adjustment” criticism, to show that the disaster is in almost every age group.
https://igorchudov.substack.com/p/uks-vaccine-hell-gets-worse-every
There Is No Pandemic – UK Column
Research by an independent statistician, who goes by the pseudonym of John Dee, appears to confirm what many have suspected since the beginning of the Covid-19 pseudopandemic; that the government narrative about the disease is a confidence trick.
John Dee looked at more than 160,000 admissions via the Emergency Department of a busy hospital. His analysis shows that, for an unnamed NHS trust, between 1 January 2021 and 13 June 2021, of the 2,102 admissions coded as Covid-19, only 9.7% (204) had any supporting diagnosis of symptomatic disease.
While focus remains firmly fixed on Covid-19, a second health crisis is quietly emerging in Britain. Since the beginning of July, there have been thousands of excess deaths which were not caused by coronavirus.
According to health experts, this is highly unusual for the summer. Although excess deaths are expected during the winter months, when cold weather and seasonal infections combine to place pressure on the NHS, summer generally sees a lull.
According to the Office for National Statistics (ONS) since July 2, there have been 9,619 excess deaths in England and Wales, of which 48 per cent (4,635) were not caused by Covid-19.
Christopher Chope MP raises the figures for damage caused by Covid-19 vaccines in Parliament: “There’s a lot more damage being done to our citizens as a result of Covid-19 vaccinations than in any other vaccination program in history.”
Backup mirrors:
Here is statement from Dr. Malcolm Kendrick which deserves to be archived in full. Links to the to original post and archive can be found below.
Thank you to the many people who have e-mailed me recently and asked if I have been silenced. I have not. I have had letters from Public Health England and the General Medical Council, informing me that I was under investigation for daring to question anything about COVID19, particularly vaccines.
The good news is the investigations ended up nowhere, and were closed down. I have also had irate phone calls from doctors, telling me that I must not question vaccination and suchlike. This has been somewhat wearing and has caused me to remain silent for a while and think about things.
However, I do know how to play the medical regulations game. Don’t make a statement you cannot reference from a peer-reviewed journal. Don’t give direct advice to people over the internet. Provide facts, and do not make statements such as ‘vaccines are killing thousands of people.’ Or suchlike.
Not that I ever would. My self-appointed role within the COVID19 mayhem, was to search for the truth – as far as it could be found – and to attempt to provide useful information for those who wish to read my blog.
The main reason for prolonged silence, and introspection, is that I am not sure I can find the truth. I do not know if it can be found anymore. Today I am unsure what represents a fact, and what has simply been made up. A sad and scary state of affairs.
This is not just true of the mainstream and the mainstream media, which has simply decided to parrot all Government and WHO statements without any critical engagement…or thought. For example, the BBC intones that ‘In the last day, fifty people died within twenty-eight days of a positive COVID19 test…’ Or a hundred, or six. What the hell is this supposed to mean? It means nothing, it is the very definition of scientific meaninglessness.
Especially when it seems that very nearly a half of those admitted to hospital with COVID19 were not admitted to hospital with COVID19. They were admitted with something else entirely, then had a positive test whilst in hospital. In short, they were not admitted to hospital with COVID19, and almost certainly did not die of COVID19. They died with a positive COVID19 test. With, not of.
But the misinformation is equally a problem for those on the other side. Claims are made for the benefits of Ivermectin and hydroxychloroquine that simply do not stand up to scrutiny. Yes, I believe both drugs may provide some benefit, but not the claimed 90% reduction in deaths that I have seen trumpeted.
So, I have given up on COVID19. It is a complete mess, and I feel that, without being certain of the ground under my feet, I have nothing to contribute. I too am in danger of starting to make statements that are not true.
However, before leaving the area entirely, I would like to make clear some of the things I currently believe to be true, and what I do not believe to be true. If this is of any assistance to anyone. Very little is referenced, because I can very easily find a contradictory reference to any reference I provide. For each fact, there is an equal and opposite fact.
1: SARS-CoV2 exists
Many people have stated, probably correctly, that the SARS-CoV2 virus has never been fully isolated. Whatever exactly that means. Have Koch’s postulates been met? [see a bit later on] I think for viruses, Koch’s postulates are very rarely, if ever, met. Does it matter, not really.
Despite this gap I believe that SARS-CoV2 truly is a ‘new’ virus that did not exist before. So, it must have mutated somewhere, or been mutated somewhere, from another coronavirus… probably. Although it seems that SARS-CoV2 does not mutate. Instead, it creates variants which, somehow or other, is a completely different process to a mutation! I have found that language in this area means little, and words are simply twisted to suit a particular narrative.
I feel it is most likely this mutation occurred within a laboratory in Wuhan during gain of function research. But I don’t suppose we will ever know. It seems unlikely to be something that the Chinese authorities are ever going to admit… ever. As a general rule, the more fervently, and angrily, the Chinese state denies something – the more likely it is to be true.
This is a special case of a general rule that I modestly call the ‘Kendrick reverse meaning law.’ Which developed from P.G. Wodehouse’s observation that ‘When an Englishman says ‘trust me’ it is time to start counting the spoons.’
This reverse meaning was seen clearly when Matt Hancock (UK Health Secretary at the time) stated that ‘Right from the start we’ve tried to throw a ring of steel around our care homes.’ Which actually meant that ‘Right from the start we threw care homes under a bus.’ Unless, what he actually meant was that the ring of steel was put up to stop care home residents escaping. ‘Halt, who goes there….’ Sound of heavy machine gun fire, whistles screeching, attack dogs baying at the leash. ‘Go for the Zimmer frames, that should bring them down.’
2: SARS-CoV2 is generally more deadly than influenza
Of course, SARS-CoV2 is most certainly not deadlier than the influenza epidemic of 1918-19. Which is estimated to have wiped out 2% of the entire world’s population. It is probably not more deadly than the 1957 epidemic, or the 1967 influenza epidemic. But it seems more deadly than anything in the last forty years, or so. So, a bit more deadly than most influenzas that sweep through humanity every year, or so. Give or take.
Currently, SARS-CoV2 is reckoned to have killed four and half million people across the Globe. Which is 0.07% of the world’s population. However, there is an immediate problem here. With influenza, we count for one year, then start again the next year. With COVID19 we have just kept on counting, adding this year figures to last years, and so on!
Eventually, therefore, assuming COVID19 comes and goes like the flu, and we just keep on counting without end, it will end up killing a hundred million. Making it the deadliest virus ever. Far worse than any influenza? At the current rate this will take another thirty years, or so. Within one thousand six hundred and sixty-six years it will have killed everyone. Of course, there will have been a few billion replacement humans created during that time.
What is far more important is to know the infection fatality rate (IFR)? That is, what percentage of those infected with SARS-CoV2 will die? This, I am afraid, we are never going to know, as the definition of what the word ‘infected’ means has flipped this way and that and can never be pinned down.
Does it mean a positive test? Does it mean a positive test plus symptoms? [Which used to be called a ‘case’] Does it mean something else. What does infected actually mean…
Here, I defer to the Master – Lewis Carroll:
‘When I use a word,” Humpty Dumpty said in rather a scornful tone, “it means just what I choose it to mean — neither more nor less.”
“The question is,” said Alice, “whether you can make words mean so many different things.”
“The question is,” said Humpty Dumpty, “which is to be master – – that’s all.”
Accepting that no-one will define what COVID19 infection actually means, I believe the infection fatality rate is, (using previous used definitions) settling at around 0.15%. At least it was last time I looked. This was never enough to justify the panicked actions that have taken place around the globe. Never.
3: The figures make no sense – and never will
One of the central problems here, form which all other problems flow, is that the PCR (polymerase chain reaction) test is the test against which the PCR test itself is tested. We have nothing better. So, we are completely reliant on it being accurate. However, we cannot know how accurate it truly is, because there is no test against which to compare it.
I mentioned Koch’s postulates earlier. These are the tests which can prove if a ‘micro-organism’ is actually causing the disease. The ultimate gold standard:
The microorganism must be found in abundance in all organisms suffering from the disease, but should not be found in healthy organisms. The microorganism must be isolated from a diseased organism and grown in pure culture. The cultured microorganism should cause disease when introduced into a healthy organism. The microorganism must be re-isolated from the inoculated, diseased experimental host and identified as being identical to the original specific causative agent. And good luck with all of that. The truth is that these postulates can work for bacteria, but not really for viruses. Because it is very difficult to meet them. I am not sure if they have ever been truly met for any virus.
On the matter of finding out if the virus is truly present, in anyone diagnosed with COVID19, here is a letter that was published in the BMJ in October last year
‘We are told that the virus is everywhere – in the air, in our breath, on fomites, trapped in masks – yet public health authorities seem not to be in possession of any cultivable clinical samples of the offending pathogen.
In March 2020, the World Health Organisation instructed authorities not to look for a virus but to rely instead on a genome test, the RT-PCR, which is not specific for SARS-CoV-2 (1) (2).
A Freedom of Information request to Public Health England about cultivable clinical samples or direct evidence of viral isolation has no information and refers to the proxy RT-PCR test, quoting Eurosurveillance (3).
Eurosurveillance states: “Virus detection by reverse transcription-PCR (RT-PCR) from respiratory samples is widely used to diagnose and monitor SARS-CoV-2 infection and, increasingly, to infer infectivity of an individual. However, RT-PCR does not distinguish between infectious and non-infectious virus. Propagating virus from clinical samples confirms the presence of infectious virus but is not widely available (and) requires biosafety level 3 facilities” (4).
The CDC admits that, “no quantified virus isolates of the 2019-nCoV are currently available”, and used a genetically modified human lung alveolar adenocarcinoma cell culture to, “mimic clinical specimen”(5).
It appears, therefore, that we have public health bodies without clinical samples, a test which is non-specific and does not distinguish between infectivity and non-infectivity, a requirement for biosafety level 3 facilities to even look for a virus, yet we are led to believe that it is up all our noses.
So, where is the virus?’
(1) https://www.who.int/publications/i/item/10665-331501
(2) https://www.bmj.com/content/369/bmj.m2420/rr-5
(3) https://www.whatdotheyknow.com/request/679566/response/1625332/attach/ht…
(4) https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2020.25.32…
(5) https://www.fda.gov/media/134922/download 1
After reading this, do I still think SARS-CoV2 exists? Yes, I do. I firmly believe that I watched people dying of it, from it. They died in a way I have never seen people do so before, and I have seen a lot of people die. They seemed quite well, then suddenly their oxygen sats dropped like a stone – they still seemed okay otherwise – then they died. The end.
Very strange, and rather disturbing. I started slipping an oxygen saturation monitor onto my finger from time to time. Just in case. 99% is my average reading, if you are interested. It never dropped.
However, getting back to the testing. If you truly want to confirm the presence of a virus in a sample, you need to send it to biosafety level 3 facilities to isolate it, grow it (not really the correct word for a virus), and suchlike. This is never done in the clinical setting.
You could argue that if you wait for antibodies to develop, you can ‘prove’ that someone was infected, or not, and thus work out how accurate the PCR test has been retrospectively. Perhaps…
I speak as someone who needed seven Hepatitis B vaccinations before I produced any detectable antibodies. Did I have immunity after the first six, or not? Am I someone who simply does not make many antibodies, but still have immunity through other mechanisms? Do others simply not produce antibodies, or their level drops so fast, that they effectively disappear?
Yes, serological testing (looking for antibodies), has its own very significant problems.
‘Serological tests for SARS-CoV-2 have accuracy issues that warrant attention. They measure specific antibody responses which may take some weeks to develop after disease onset reducing the sensitivity of the assay. If blood samples were collected during the early stage of the infection, they may produce false negative results. They do not directly detect the presence of the virus. Further, antibodies may be present when SARS-CoV-2 is no longer present giving false positive case diagnosis.’ 2
In reality, we are relying on a PCR test to diagnose SARS-CoV2 infection, the accuracy of which is entirely dependent on believing that the test is accurate. Yes, that is the route to madness.
At present, in the UK, we are doing about one million tests a day 3.
We are getting about thirty thousand ‘positive’ results. Or, about 3% positive. How many of these are truly positive? Well, you can take a wild guess on that one. At one point, the CDC stated that 30% of the PCR tests were false positives. A ‘false positive’ means that test says you have the disease, when you do not. [A false negative informs you that you do not have the disease, when you do] 4.
The thirty per cent cannot be the case currently, because that would mean if you did one million tests, you would get more than three hundred thousand false positives. Instead we are getting thirty thousand, which means that it is impossible for the false positive rate to be higher than three per cent.
So, what is the true rate? Well, if is three percent, then virtually every single positive test is a false positive test. [Three per cent of one million is thirty thousand] Which would mean that no-one in the UK currently has COVID19, and everything we are doing is completely pointless. It also means that people admitted to hospital with COVID19 do not have the disease, they are suffering from, and dying from, something else with a false positive COVID19 false test stamped on their forehead.
Is it possible that no-one actually is infected with SARS-CoV2? Well, it is certainly not impossible. Here is a graph of overall mortality (risk of dying of anything) from England. These figures, unlike most others, are pretty much fully reliable. Someone is either dead, or they are not. It is a difficult thing to get wrong, or manipulate. There can be some delay in registering a death, but this is not normally a major issue.
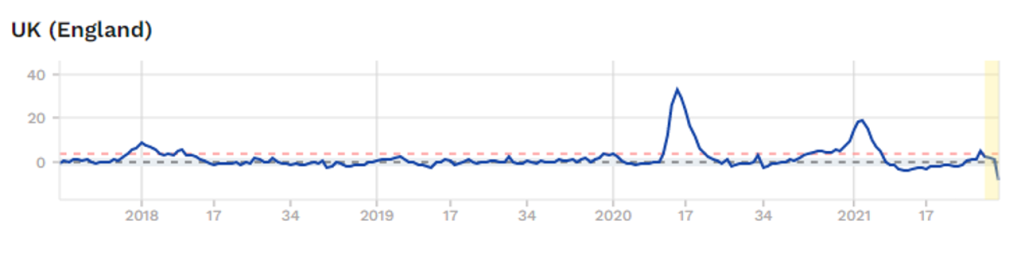
The graph starts in last quarter 2017. As you can see, a spike in overall mortality in Spring 2020, A spike in Winter 2020/21. Currently, no excess mortality at all. So, if COVID19 is infecting hundreds of thousands of people each week, it is not showing up as any excess deaths… at all 5.
Does this mean that COVID19 has gone, and we are rushing around panicking about false positive tests? Or is it still here? Still here I think… but who knows… who knows.
This is the main reason I have given up. I just don’t know what to believe – apart from overall mortality figures. The figures are spun and massage, twisted and mangled.
Another reason why I have given up trying to make any sense of COVID19 is the enormous differences in overall mortality seen in countries that are virtually identical in life expectancy, healthcare systems, actions taken against COVID19 etc. etc.
Afters studying the figures from England, I looked at the figures from Northern Ireland.
Both countries [yes, Northern Ireland is not actually a separate country, it is part of the UK] did almost exactly the same things when it came to COVID19. They both have the National Health Service, they are as close to each other as can be – in terms of COVID19, and most other things. Here is the graph of overall morality for Northern Ireland.
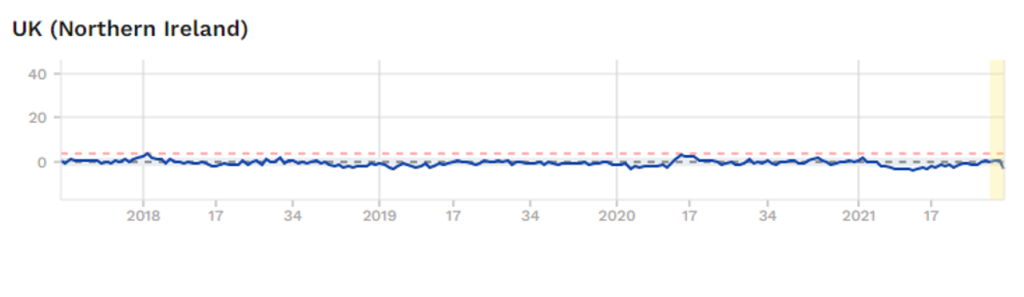
Which means that something very dramatic happened in England, with regard to COVID19? Yet nothing happened in Northern Ireland. This, to me, is fascinating, although I cannot explain it. However, I know that if you were able explain why these two graphs are so weirdly different, you will be unearthing some critical truths with regard to COVID19.
Of course, no-one is remotely interested in such anomalies. Instead, they point to a country like Norway and say – ‘Look how well they did with their rapid lockdown, and preventing people crossing the border’. No-one points to Northern Ireland and says, ‘look how well they did with all their….’ All their what? All their doing exactly the same as England.
Yes, Northern Ireland does not fit with the approved narrative, so it is ignored. Anything that does not fit with the mask wearing, social isolating, vaccination will save the world narrative is simply ignored.
Or it is shouted down or censored by the self-appointed Fact-checkers. Those mighty intellects who can determine what is true, and what is not. It was thoughtful of them to descend from Mount Olympus to mingle amongst feeble minded humanity and tell us what we should, and should not, be thinking. We must all be eternally grateful that the ‘Truth Gods’ now live amongst us, to firmly inform us all what, and how, we should be thinking. And shut us down if we veer from the official narrative.
Anyway, faced with a situation where there are almost no facts that can be relied upon, from anywhere, I have officially removed myself from all discussions on the matter of COVID19.
Instead, I shall return to other areas where, whilst the truth is constantly battered and bruised, and lying in a bruised heap the corner, it is still breathing … just about alive. Sometimes it is capable of weakly raising its head and whispering quietly into my ear. I shall let you know what it says.
1: https://www.bmj.com/content/370/bmj.m3379/rr-2
2: https://systematicreviewsjournal.biomedcentral.com/articles/10.1186/s13643-021-01689-3
3: https://coronavirus.data.gov.uk/?_ga=2.38943459.111756282.1590603430-1775824629.1590603430
4: https://www.bmj.com/content/373/bmj.n1411/rr
5: https://www.euromomo.eu/graphs-and-maps/
https://drmalcolmkendrick.org/2021/09/03/i-have-not-been-silenced/
The real-world study includes data on positive Covid PCR test results between May and July 2021 among more than a million people who had received two doses of Pfizer or AstraZeneca vaccine.
Protection after two shots of Pfizer decreased from 88% at one month to 74% at five to six months.
For AstraZeneca, the fall was from 77% to 67% at four to five months.
http://archive.today/2021.08.25-105339/https://www.bbc.com/news/health-58322882
Excess deaths have not been this high since the week ending Feb 19, when 2,182 extra deaths were registered – 18.8 per cent above the pre-2020 five-year average.
Although some of the increase in excess deaths can be explained by the recent rise in deaths involving Covid, most were not linked to the virus.
Kevin McConway, emeritus professor of applied statistics at The Open University, said: “These excess deaths can’t all be explained by deaths of people who had Covid-19. In the most recent week, for England and Wales there were 1,270 more deaths than the five-year average – that’s 14 per cent higher than that average.
…Deaths in private homes have been well above the 2015-19 average almost every week since April last year. Before Covid, around a quarter of deaths occurred at home but that has since risen to one third, according to research by the King’s Fund.
What [covid jabs] won’t do, according to an increasing body of evidence, is prevent you from being a carrier and thus a danger to others. This somewhat defeats the whole point – and is certainly the only reason international travel has resumed of late.
Last week, in news that hasn’t got nearly enough airtime, Public Health England said in a statement: “Some initial findings […] indicate that levels of virus in those who become infected with Delta having already been vaccinated may be similar to levels found in unvaccinated people. This may have implications for people’s infectiousness, whether they have been vaccinated or not.”

This means that whilst vaccination may reduce an individual’s overall risk of becoming infected, once they are infected there is limited difference in viral load (and Ct values) between those who are vaccinated and unvaccinated. Given they have similar Ct values, this suggests limited difference in infectiousness.

Schools are not spreading Covid, according to an official study that has boosted hopes that the return to class will not trigger an autumn surge in infections.
Pupils sent home in class bubbles were highly unlikely to pass on the virus to their parents even when they did pick up it from a fellow pupil, the research found.
https://www.thetimes.co.uk/article/75136706-f171-11eb-8f01-2c678acbb979
25 CYP died of SARS-CoV-2 during the first pandemic year in England, equivalent to an infection fatality rate of 5 per 100,000 and a mortality rate of 2 per million. Most had an underlying comorbidity, particularly neurodisability and life-limiting conditions. The CYP who died were mainly >10 years and of Asian and Black ethnicity, compared to other causes of the death, but their absolute risk of death was still extremely low.