A senior epidemiologist who advised the government during the coronavirus pandemic claims he was told to “correct” his views after he criticised what he thought was an “implausible” graph shown at an official briefing.
Professor Mark Woolhouse has also apologised to his daughter, whose generation “has been so badly served by mine”, and believes that closing schools was “morally wrong”.
The Edinburgh University academic is deeply critical of the use of lockdown measures and says “plain common sense” was a “casualty of the crisis”.
Speaking to Sky News, Prof Woolhouse seemed concerned about a possible “big-brother” approach to the control of information about COVID.He says he was told to watch what he was saying following a briefing given by Chief Scientific Adviser (CSA) Sir Patrick Vallance on 21 September 2020.
Cases
COVID-19 case numbers are not a useful metric unless tests are accurate and you know how testing is being conducted. Current evidence shows that case counts increase as testing increases; current tests have high false positive and false negative rates; and a positive test does not mean someone is sick.
Browse the articles related to this topic below.
Join our community on Guilded.
More than half of new ‘Omicron patients’ are actually people being treated in hospital for a different reason
These people are in hospital for physical injuries such as broken bones, heart attacks, or even routine care
Ministers are keeping a close eye on Covid hospital admissions as they weigh up imposing more restrictions
Two-thirds of new Covid hospital patients in England were actually admitted for a different ailment, MailOnline’s analysis of NHS data suggests – as a growing number of studies show Omicron is much milder than Delta.
In the two weeks to December 21, hospitals in England recorded 563 new coronavirus inpatients — the majority of which are believed to be Omicron now that the variant is the country’s dominant stain.
But just 197 (35 per cent) were being primarily treated for Covid, with the remaining 366 (65 per cent) only testing positive after being admitted for something else.
The Zoe Covid study team has been tracking the pandemic using feedback from the general public, and estimates half of people with cold-like symptoms actually have Covid.
They describe an “explosion” of Covid cases over the last week, driven by the new Omicron variant.
http://archive.today/2021.12.24-093600/https://www.bbc.com/news/health-59768366
Dec 10 (Reuters) – Most of the 43 COVID-19 cases caused by the Omicron variant identified in the United States so far were in people who were fully vaccinated, and a third of them had received a booster dose, according to a U.S. report published on Friday.
The U.S. Centers for Disease Control and Prevention (CDC) said that of the 43 cases attributed to Omicron variant, 34 people had been fully vaccinated. Fourteen of them had also received a booster, although five of those cases occurred less than 14 days after the additional shot before full protection kicks in.
While the numbers are very small, they add to growing concerns that current COVID-19 vaccines may offer less protection against the highly transmissible new variant.
Data on confirmed Covid cases in England show how the Omicron variant is already taking hold in the country
Proportion of confirmed positive tests that didn’t detect the spike protein increased from 0.1% to 0.3%
One scientist said it equates around 60 more cases with hallmark than usual, suggesting Omicron infections
Comes as R rate spirals from less than one to 3.5 in South Africa’s Omicron epicentre Gauteng province
Lead UK epidemiologist says Omicron infections likely appear mild because of immunity from past infections
WHO officials suggested on Thursday that Covid cases were milder in those who caught the Omicron strain
The five most vaccinated states in the United States—Vermont, Rhode Island, Maine, Connecticut and Massachusetts—are all experiencing surges in new COVID-19 cases, as the Biden administration urges people over 50 to get their booster jabs.
Vermont, which is the most vaccinated state, with 73 percent of its population fully jabbed, saw an 18 percent rise in new daily COVID cases over the last 14 days before November 24, according to New York Times data.
Terrified Indigenous Australians are being taken by army to quarantine facilities
At-risk remote Aboriginal communities have been hit by a new Covid outbreak
Authorities have started moving positive cases and contacts to Howard Springs
Elder from Larrakia country claimed people were ‘being taken against their will’
But Indigenous man quarantining in facility said everyone is being treated well
Binjari and Rockhole residents aren’t allowed to shop or even go for a walk
It is currently the strictest lockdown on earth with hundreds trapped at home
High COVID-19 vaccination rates were expected to reduce transmission of SARS-CoV-2 in populations by reducing the number of possible sources for transmission and thereby to reduce the burden of COVID-19 disease. Recent data, however, indicate that the epidemiological relevance of COVID-19 vaccinated individuals is increasing.
…The US Centres for Disease Control and Prevention (CDC) identifies four of the top five counties with the highest percentage of fully vaccinated population (99.9–84.3%) as “high” transmission counties.
These prognosticators of doom have been wrong time after time after time. And not just a little bit wrong – epically wrong, all while morally condemning their more accurate opponents. As cases rose in early July, in the run-up to England’s full reopening on July 19, restrictions advocates said that it was inevitable we would reach 100,000 cases per day. Keir Starmer released a video statement in which he declared that “Boris Johnson’s recklessness means we’re going to have an NHS summer crisis. The Johnson Variant is already out of control.” A set of academics wrote a letter to The Lancet condemning the reopening as a “dangerous and unethical experiment”.
One of the UK’s leading childhood health experts has said there is not enough evidence to support vaccinating children against Covid, and the body that will make the decision on whether to jab under-18s has indicated it will take a cautious approach.
Prof Calum Semple, a member of the Scientific Advisory Group for Emergencies (Sage), said there was “rock-solid data” to show that the risk of severe harm to children from Covid was “incredibly low”.
Professor Robert Dingwall said children may be “better protected by natural immunity generated through infection than by asking them to take the ‘possible’ risk of a vaccine”.
…On Wednesday, Prof Dingwall, a social scientist who sits on a subcommittee of the Scientific Advisory Group for Emergencies (Sage) as well as on the JCVI, spoke out, saying the “risk/benefit for teenagers must be firmly established” before any decisions were taken.
In a detailed Twitter thread, he said: “Teenagers are at intrinsically low risk from Covid. Vaccines must be exceptionally safe to beat this. Given the low risk of Covid for most teenagers, it is not immoral to think that they may be better protected by natural immunity generated through infection than by asking them to take the possible risk of a vaccine.”
Admissions have failed to sky-rocket – and it’s time ministers took their own advice about learning to live with the virus
Innova tests’ performance not proven and they should be returned to manufacturer or thrown in bin, says FDA
The US Food and Drug Agency (FDA) has raised significant concerns about the rapid Covid test on which the UK government has based its multibillion-pound mass testing programme.
In a scathing review, the US health agency suggested the performance of the test had not been established, presenting a risk to health, and that the tests should be thrown in the bin or returned to the California-based manufacturer Innova.
…In its report, the agency accused the company of “false or misleading” estimates of the clinical performance of certain configurations of the test, saying the estimates did not accurately reflect the performance of the diagnostic devices during clinical studies.
Hospitals have been told to change the way they collect data on patients infected with coronavirus to differentiate between those actually sick with symptoms and those who test positive while seeking treatment for something else.
The move would reduce the overall number of patients in hospital for coronavirus as until now data from hospitals has included all patients who tested positive for Covid-19, regardless of whether they had symptoms or not.
https://www.independent.co.uk/news/health/coronavirus-hospitals-nhs-england-data-b1862804.html
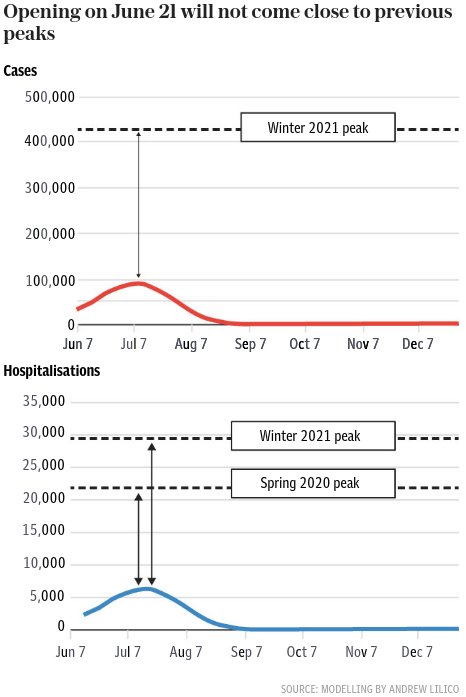
Do we risk swamping the NHS with Covid-19 cases if the government proceeds with Step 4 on time on June 21st? In the Spring of 2020, there were about 22,000 Covid cases per week admitted to hospital, at the peak.
In January 2021 there were about 29,500 at that peak.
Neither of those occasions produced any British equivalent of the distressing scenes we recently saw in India where hospitals ran out of resources and turned sick people away, with relatives forced to watch their loved-ones die, untreated, in hospital car parks.
The NHS was not swamped, in that sense, on those occasions. And we should not understate how important it was that it was not.
Nearly 40 per cent of recently registered Covid deaths in England and Wales were people who died primarily from another condition, latest figures from the Office for National Statistics (ONS) show.
Out of 107 Covid deaths registered in the week ending May 21, just 66 had coronavirus recorded as the underlying cause of death, 61.7 per cent.
Britain recorded no new deaths within 28 days of a positive COVID-19 test on Tuesday.
The last time Britain recorded no deaths was in March 2020, before the country had entered its first lockdown. The figure on Tuesday relates to how many deaths have been reported and it comes after a national holiday on Monday – a factor which has in the past skewed the data.
…Britain’s overall death toll from the pandemic stands at 127,782 and is the fifth highest in the world, according to Johns Hopkins University data.
https://www.reuters.com/world/uk/uk-reports-no-new-covid-19-deaths-3165-new-infections-2021-06-01/
The CDC has put new policies in place which effectively created a tiered system of diagnosis. Meaning, from now on, unvaccinated people will find it much easier to be diagnosed with Covid19 than vaccinated people.
Person A has not been vaccinated. They test positive for Covid using a PCR test at 40 cycles and, despite having no symptoms, they are officially a “covid case”.
Person B has been vaccinated. They test positive at 28 cycles, and spend six weeks bedridden with a high fever. Because they never went into a hospital and didn’t die they are NOT a Covid case.
Person C, who was also vaccinated, did die. After weeks in hospital with a high fever and respiratory problems. Only their positive PCR test was 29 cycles, so they’re not officially a Covid case either.
Plans for Covid passports have been significantly scaled back as government ministers privately question whether they should be adopted at all, The Telegraph understands.
