- Misinformation #1: Natural immunity offers little protection compared to vaccinated immunity
- Misinformation #2: Masks prevent Covid transmission
- Misinformation #3: School closures reduce Covid transmission
- Misinformation #5: Young people benefit from a vaccine booster
- Misinformation #6: Vaccine mandates increased vaccination rates
- Misinformation #7: Covid originating from the Wuhan Lab is a conspiracy theory
- Misinformation #8: It was important to get the 2nd vaccine dose 3 or 4 weeks after the 1st dose
- Misinformation #8: It was important to get the 2nd vaccine dose 3 or 4 weeks after the 1st dose
- Misinformation #9: Data on the bivalent vaccine is “crystal clear”
- Misinformation #10: One in five people get long Covid
Herd Immunity
Evidence shows we may already have developed herd immunity to COVID-19 and can continue to manage it through herd immunity.
Professor Sunetra Gupta explains herd immunity in the linked video.
Browse the articles related to this topic below.
Join our community on Guilded.
It is more than a rebuke to Medley and the modellers though. This pandemic began, for many, with an announcement from Imperial College, whose study predicted 500,000 deaths if we did nothing. We locked down and never tested the prediction.
This time, in the face of what the public saw as dire predictions, we didn’t lock down and the apocalypse never came. The unspoken — and sometimes spoken — implication is clear: are we all fools?
The Prime Minister has talked of giving Whitty a knighthood — but after that reckless and irresponsible performance, the Chief Medical Officer deserves the boot.
At a stroke, he inflicted spectacular damage on our economy, particularly the hospitality sector which makes over a quarter of its profits in this period, and which has already taken a termendous battering during the pandemic.
…The irony is that if the most lurid forecasts of the lockdown addicts are realised, with the pandemic reaching every household, then all those oppressive measures they cherish most — such as social distancing, bans on large gatherings, venue closures and vaccine passports — will be largely useless.
…And in fact it would be worse than meaningless: it would be counter-productive. Lockdown directly undermines the fight against the virus by preventing the spread of naturally acquired Covid immunity in the population.
Arguments to vaccinate children as young as five against Covid are ‘scientifically weak’, British experts claimed today after the US moved closer to jabbing infants.
…Professor David Livermore, a medical microbiologist at the University of East Anglia told MailOnline: ‘Vaccinating children to protect adults via herd immunity is ethically dubious and is scientifically weak.’
…Professor Russell Viner, a pediatrician and member of the UK Government’s scientific advisory group SAGE, said it was crucial the UK does not ‘rush to a decision’ in the wake of the announcement in the US.
The authorities are literally going against the science and lying to victims of Covid in order to avoid creating a benefit that others might seek out at a potential risk. Except that they themselves are responsible for creating the restrictive system from which people are now literally seeking out infection to find relief – if only to acquire a health pass good for six months so they’re able to access everyday venues and basic freedoms.
Dr. Philip McMillan interviews vaccine developer Geert Vanden Bossche and Robert Malone MD, inventor of mRNA vaccine platform.
Interview highlights
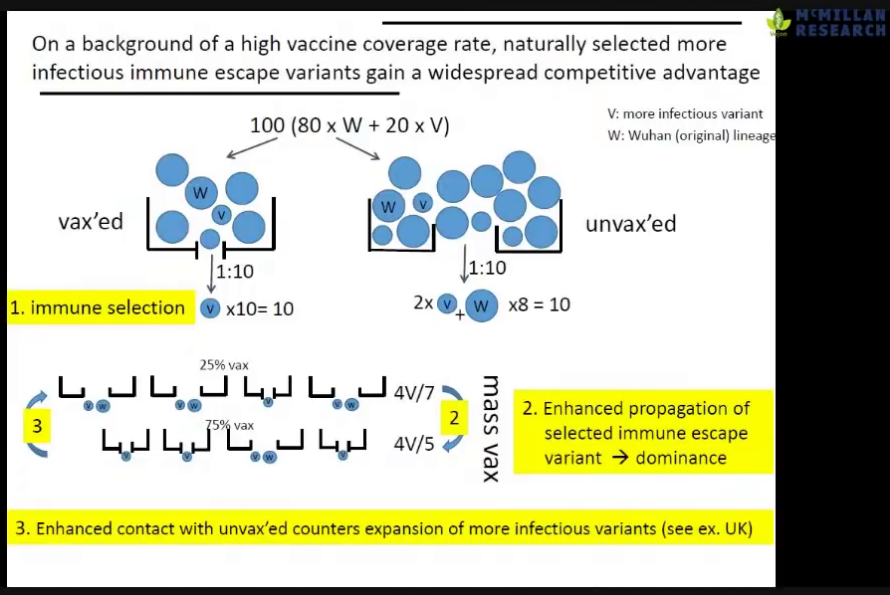
- Geert Vanden Bossche (GV) at 17m: Massive surges of the infection rates, especially in countries with an aggressive mass-vaccination policy, was predictable.
- Robert Malone (RM) at 23m: The Israeli data is a concern: we are seeing signs that the durability of the [Pfizer vaccine] is very poor.
- RM at 26m: The vaccinated are a higher risk of becoming superspreaders because they’re replicating virus at the same or higher levels than the unvaccinated but they feel better.
- GV at 28m: The effect of mass-vaccination is an ideal breeding-ground for more infections spread. However, if still have a substantial proportion that is non-vaccinated, you will see a reduction of infectious pressure.
- GV at 31m: The unvaccinated are ‘the vaccum cleaners’ who will eliminate a lot of virus from the population by mounting long-lived immunity and contribute to the reduction of infectious pressure. The vaccinated cannot contribute to the infectious pressure.
- RM at 33m: The truth is that it’s the vaccinated that are creating the risk, not the unvaccinated. The unvaccinated are serving as virus sinks. The probability of them having significant disease and death is minute. The real risk is the vaccinated who have received very focused spike proteins.
- GV at 35m: It is not a problem of individuals being vaccinated. The problem is a policy of mass-vaccination. That is how the more infections variant can adapt to the population and become dominant.
- GV at 58m: Young people are now getting the disease pretty fast because of the increased infectious pressure [due to mass-vaccination].
- RM at 1h10m: There are disincentives to asking questions about data for vaccine-enhanced replication and antibody-dependent enhancement; no-one wants fund the studies.
- GV at 1h12m: Regulators have no experience with the current situation where there are very many unknowns when deploying a new vaccine to the public.
- RM at 1h17m: The FDA is not structured to detect adverse advents and have admitted they cannot evaluate safety. Two of the top [US] regulators resigned because the FDA is no longer independent from the policy-making apparatus which exists in the Executive Branch [of US Government].
- RM at 1h24m: There is an intrinsic conflict of interest in the CDC in that it is funded to promote vaccines but also has the under-funded mission of evaluating their safety.
- RM at 1h25m: Policy recommendations together with Peter Navarro (American economist and author):
- Reserve vaccines for the high-risk population and make it available globally.
- Make early interventions [like Ivermectin and Vitamin D] widely available. Many are very effective when administered early and aggressively.
- Make home-test kits available (acknowledging that they have a bias to false positives) and make more specific tests in physicians offices.
- Address the fear by showing that currently most people are not at risk.
- GV at 1h30m: The most important thing is to reduce the infectious pressure. This is a huge threat to all those who were naturally protected, such as young people. The worst thing to do is to vaccinate the younger age groups because they are ‘the buffer’ of long-lived immunity. They are our hope for herd immunity. We will not get herd immunity from mass-vaccination.
- GV at 1h39m: We need to compare the ratio of severe disease of deaths in vaccinated and unvaccinated. We are seeing more case fatalities in the vaccinated but the numbers are not being made available.
- RM at 1h41m: There is a persistent signal in the UK data that there seems to be an excess deaths in the vaccinated and yet a relative deficit in the vaccinated. This is paradoxical.
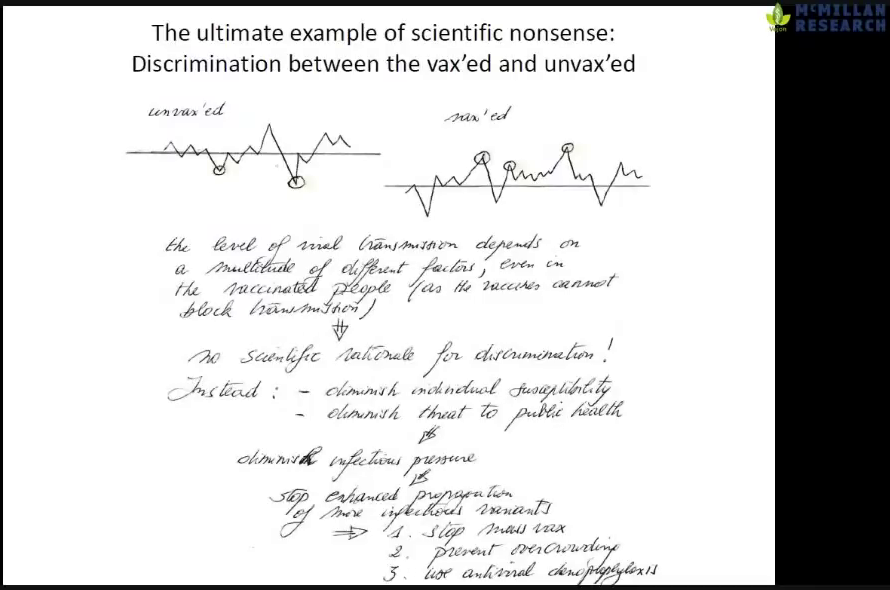
- GV at 1h47m: Discrimination against the non-vaccinated is complete scientific nonsense. We should care about susceptibility. What is relevant is how can we protect ourselves best.
Slides:
Backup mirrors:
Professor Sucharit Bhakdi: “You are now witnessing the greatest crime that England has ever committed in its history.”
Professor Sunetra Gupta of Oxford University explains herd immunity, highlighting critical details about both the concept and its relevance to the COVID-19 pandemic that are often overlooked in public discussion.
The development of immunity through natural infection is a common feature of many pathogens, and we now know that COVID-19 does not have any tricks up its sleeve to prevent this from happening. If it did, it would have posed a serious problem for the development of a vaccine.
That being said, COVID-19 belongs to a family of viruses that do not typically confer lifelong immunity against infection. Most of us have never heard of the other four ‘seasonal’ coronaviruses that are currently circulating in our communities. And yet, surveys indicate that at least 3% of the population is infected by any one of these corona cousins during the winter months each year. These viruses can – and do – cause deaths in high-risk groups or require them to receive ICU care or ventilator support. Hence, it is not necessarily true that they are intrinsically milder than the novel COVID-19 virus. And like the COVID-19 virus, the other coronas are much less virulent in the healthy elderly and younger people than influenza.
One important reason why these corona cousins do not kill large numbers of people is that, even though we lose immunity and can be reinfected, there is always a sufficient proportion of immune people within the population to keep the risk of infection low for those who might die upon contracting it. Also, all of the coronaviruses in circulation — including COVID-19 — have some features in common, which means that getting one coronavirus will probably offer some protection against the others. This is becoming increasingly clear from work in many labs, including my lab in Oxford. It is against the background of acquired immunity to COVID-19 itself, as well as its close relations, that the new virus has to operate.
It is misleading to speak of “reaching” herd immunity. Herd immunity is a continuous variable that increases as people become immune and decreases as they lose immunity or die. There is a threshold of herd immunity at which the rate of new infections begins to decrease. We do not yet have a clear idea of what this threshold is for COVID-19 as the transmission landscape includes people who are susceptible to it, people who have built up immunity to it, and people who have immunity to other coronaviruses.
Unfortunately, we do not have a good way of telling how many people have been exposed to the new virus, nor how many people were resistant to begin with. We can test for antibodies but, as with other coronaviruses, COVID-19 antibody levels decline after recovery, and some people do not make them at all. Thus, antibody levels will not answer this question. More and more evidence is accumulating that other arms of immunity, like T cells, play an important role.
Indications of the herd immunity threshold having been reached in a given location are visible in the time signatures of epidemics where death and infection curves tend to either “bend” in the absence of intervention or to stay down when interventions are relaxed (in comparison with other locations where the opposite happened). Unfortunately, we do not know how far (or close) we are to that threshold in most parts of the world. This means that we need to make public health decisions based only on limited information and do so in a constantly changing environment.
Focused Protection was initially proposed as a solution for how we could proceed in the face of such uncertainty and it remains relevant now. It suggests that we exploit the fact that COVID-19 does not cause much harm to the large majority of the population and allow those individuals to resume their normal lives, while shielding those who are vulnerable to severe disease and death. We have good information about who falls into these groups and the availability of vaccines, which offer excellent protection for vulnerable populations and guard against hospitalisable illness, provide us with the ideal setting in which to implement such a plan.
Sunetra Gupta is Professor of Theoretical Epidemiology in the Department of Zoology, University of Oxford and a member of Collateral Global’s Scientific Advisory Board.
By Professor Sunetra Gupta
28 May 2021
Backup mirrors:
The first thing to emphasise is that this fall is not the result of some special temporary factor. It isn’t that there was a week of glorious sunshine, the temporary introduction of a new set of restrictions, a sudden change in the testing rules or even the dropping out of the numbers of a previous shock that had temporarily raised numbers. It’s simply that the collective immunity we now have, through a combination of vaccines and people recovered from illness, is sufficient that, given the way we behave (eg more working from home) and given the time of year (August) the virus cannot find enough susceptible people to infect for its rate of spread to accelerate. That means, that, by definition, we have reached what is called the “herd immunity threshold” (HIT) – the collective percentage immunity, across the whole population, at which the virus can no longer sustainably spread.
Fully vaccinated people carry the same amount of Covid as the unvaccinated, scientists have found in a new study that calls into question the effectiveness of vaccine passports and changes to the NHS app.
…[E]ven the fully jabbed carry high levels of the virus if they become infected and are also more likely to be symptomatic than vaccinated people who pick up an alpha infection.
The results suggest those who are fully jabbed could be as capable of passing on Covid as the unvaccinated, although they are less likely to pick up the virus in the first place.
Some good news and some troubling news, from Professor Sucharit Bhakdi, M.D.
Oracle Films recently produced an interview with Professor Sucharit Bhakdi in collaboration with Oval Media in Germany, for an upcoming documentary.
As an aside to the interview, Dr. Bhakdi emphasised the urgent need to share the following information that has emerged from new scientific literature.
PLEASE take the time to process this presentation. Dr. Bhakdi explains clearly, based on new scientific evidence, why he believes:
* Your immune system is your best defence against SARS-CoV-2, and indeed all coronaviruses. If you have been infected, even if you experienced no symptoms at all, you are immune to all variants.
* We have already reached herd immunity.
* There is no scientific reason to vaccinate against SARS-CoV-2. There is simply no benefit and the rollout must be stopped.
Scientific literature references for Dr. Bhakdi’s presentation:
- https://www.sciencedirect.com/science/article/pii/S2352396421002036
- https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0249499
- https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciab465/6279075
- https://doi.org/10.1016/j.cell.2021.06.005
Update: On 17 July 2021, Dr. Geert Vanden Bossche posted a response to Dr. Bhakdi’s conclusions. Both agree that mass vaccination should halt but differ on the dangers of variants and whether herd immunity has been reached.

Dr. Robert Malone, inventor of the mRNA technology used in the COVID-19 injections, discusses his concerns over their safety and how concerns are censored.
- “I have been written out of history.”
- The chairman of the board of Reuters sits on the board of Pfizer.
- The conflicts of interests are overt…it’s in your face…they have no shame.
- The big thinkers in the government envy the Chinese model of government.
- The political spectrum is irrelevant [on the topic of COVID and vaccines].
- These discussions are forbidden talk so we won’t get to the truth.
- Detailed discussion on the cytotoxic effects of spike proteins and safety of the new mRNA COVID vaccines at around 40mins.
- Dr. Malone agrees with many of Dr. Mike Yeadon‘s comments, except Dr. Yeadon’s conclusion of a conspiracy.
- The figure of 70% uptake of vaccines to reach herd immunity was made up. The data isn’t known. “Somebody is just pulling it out of the air.”
- The vaccines don’t stop you from getting the virus or spreading it.
- The early trials were designed to optimise success.
- You cannot publish stuff outside of the approved memes and that means we can’t do science. People are dying because of this.
- Other treatments have been suppressed to increase uptake of the vaccine.
- The fear is bringing out social pathologies and is diminishing our ability to think.
- We’ve had rampant groupthink in the government, in the WHO and across the world.
- “I’ve never seen this level of co-ordinated crazy.”
- “I’m concerned about what’s at the other side of the tunnel.”
- The new COVID-19 vaccines are still experimental.
- “Most of us who haven’t drunk the Koolaid” say the risk of COVID to children is remarkably low and the risk of vaccines is not nothing.
- There is no logic in vaccinating children, adolescents and young adults. There are some risk and they’re not trivial.
Source links can be found at The Last American Vagabond.
Flu could be a “bigger problem” than Covid-19 this winter, the deputy chairman of the Joint Committee on Vaccination and Immunisation (JCVI) has warned.
Professor Anthony Harnden told BBC 4’s Today programme: “I will emphasise that actually flu could be potentially a bigger problem this winter than Covid.
“We’ve had a very, very low prevalence of flu for the last few years, particularly virtually nil during lockdown, and we do know that when flu has been circulating in very low numbers immunity drops in the population, and it comes back to bite us. So, flu can be really, really important this winter.”
SARS-CoV-2 spike antigen-specific IgG and IgA elicited by infection mediate viral neutralization and are likely an important component of natural immunity, however, limited information exists on vaccine induced responses. We measured COVID-19 mRNA vaccine induced IgG and IgA in serum serially, up to 145 days post vaccination in 4 subjects. Spike antigen-specific IgG levels rose exponentially and plateaued 21 days after the initial vaccine dose. After the second vaccine dose IgG levels increased further, reaching a maximum approximately 7–10 days later, and remained elevated (average of 58% peak levels) during the additional >100 day follow up period. COVID-19 mRNA vaccination elicited spike antigen-specific IgA with similar kinetics of induction and time to peak levels, but more rapid decline in serum levels following both the 1st and 2nd vaccine doses (<18% peak levels within 100 days of the 2nd shot). The data demonstrate COVID-19 mRNA vaccines effectively induce spike antigen specific IgG and IgA and highlight marked differences in their persistence in serum.
https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0249499
Dr. Hodkinson, here to discuss the dangers of the COVID-19 vaccines, the possibility of infertility, and the very real concerns about the vaccine-induced spike proteins and what new scientific research is clearly suggesting about their risks to your health.
But the time has come when the hard choices are looming closer. If we don’t want this Covid crisis to last forever, we need some new simple, guidelines: No jab, no job; no jab, no access to NHS healthcare; no jab, no state education for your kids. No jab, no access to pubs, restaurants, theatres, cinemas, stadiums. No jab, no entry to the UK, and much else.
https://www.independent.co.uk/voices/antivaxxers-vaccine-coronavirus-nhs-b1849437.html
Unlocked Exclusive — in a hard-hitting interview, retired NHS pathologist Dr John Lee discusses the government’s response to the pandemic, analyses why proven scientific procedures were abandoned, makes the case for ending Lockdown now, and asks the question most doctors are unable to discuss in public. Covid-19: is the cure worse than the disease?
Backup mirrors:
https://www.facebook.com/unlockedunitedkingdom/videos/506787697359395/
I won’t have been the only parent concerned by news last week that the Pfizer vaccine may be approved for use on children as early as June and potentially rolled out to school pupils from September. Healthy children are at almost no serious risk from Covid-19 – the recovery rate for this age group has been calculated at over 99.99 per cent. The argument that children should have the vaccine is not based on a belief that they need or benefit from it but on the logic that it would be good for our communities at large if children were jabbed. In short, those advocating it assume that children have an obligation to protect adults.
It’s worth noting that the UK Government has granted immunity from liability for harms to all Covid-19 vaccine manufacturers. Can we really ask children to accept a greater risk than the manufacturers themselves are prepared to live with?
https://www.telegraph.co.uk/news/2021/05/03/healthy-children-simply-do-not-need-covid-jab
The open letter states that “a good society cannot be created by an obsessive focus on a single cause of ill-health” and states all restrictions should be lifted in June on the final date in Prime Minister Boris Johnson’s ‘roadmap’ out of lockdown. Masks should no longer be worn by schoolchildren after May 17, say the scientists – and they warn the damage to society will be too great if the current Covid control measures continue beyond the June roadmap date.
Vaccine passports should also be scrapped along with mass community testing, they say.
Instead, the government should focus on targeted testing, creating better incentives for staying home if ill and basic hygiene measures, such as handwashing and surface cleaning.
Signatories (in alphabetical order)
Professor Ryan Anderson, Translational Science, Medicines Discovery Catapult
Dr Colin Axon, Mechanical Engineering, Brunel University
Professor Anthony Brookes, Genomics and Bioinformatics, University of Leicester
Professor Jackie Cassell, FFPH, Deputy Dean, Brighton and Sussex Medical School
Professor Angus Dalgleish, FRCP, FRCPath, FMedSci, Oncology, St George’s, University of London
Professor Robert Dingwall, FAcSS, HonMFPH, Sociology, Nottingham Trent University
Professor Sunetra Gupta, Theoretical Epidemiology, University of Oxford
Professor Carl Heneghan, MRCGP, Centre for Evidence Based Medicine, University of Oxford
Professor Mike Hulme, Human Geography, University of Cambridge.
Dr John Lee – formerly Pathology, Hull York Medical School
Professor David Livermore, Medical Microbiology, University of East Anglia.
Professor Paul McKeigue Genetic Epidemiology and Statistical Genetics, University of Edinburgh
Professor David Paton, Industrial Economics, University of Nottingham
Emeritus Professor Hugh Pennington, CBE, FRCPath, FRCP (Edin), FMedSci, FRSE, Bacteriology, University of Aberdeen
Dr Gerry Quinn, Biomedical Sciences, University of Ulster
Dr Roland Salmon, MRCGP, FFPH, former Director of the Communicable Disease Surveillance Centre (Wales).
Emeritus Professor John Scott, CBE, FRSA, FBA, FAcSS, Sociology, University of Essex
Professor Karol Sikora, FRCR, FRCP, FFPM, Medicine, University of Buckingham
Professor Ellen Townsend, Psychology, University of Nottingham
Dr Chao Wang, Health & Social Care Statistics, Kingston University and St George’s, University of London,
Professor John Watkins, Epidemiology, Cardiff University
Professor Lisa White, Modelling and Epidemiology, University of Oxford.
A year ago, there was no evidence that lockdowns would protect older high-risk people from Covid-19. Now there is evidence. They did not.
With so many Covid-19 deaths, it is obvious that lockdown strategies failed to protect the old. Holding the naïve belief that shutting down society would protect everyone, governments and scientists rejected basic focused protection measures for the elderly. While anyone can get infected, there is more than a thousand-fold difference in the risk of death between the old and the young. The failure to exploit this fact about the virus led to the biggest public health fiasco in history.