Two infectious-disease experts I spoke with believe that the number of deaths attributed to covid is far greater than the actual number of people dying from covid. Robin Dretler, an attending physician at Emory Decatur Hospital and the former president of Georgia’s chapter of Infectious Diseases Society of America, estimates that at his hospital, 90 percent of patients diagnosed with covid are actually in the hospital for some other illness.
“Since every hospitalized patient gets tested for covid, many are incidentally positive,” he said. A gunshot victim or someone who had a heart attack, for example, could test positive for the virus, but the infection has no bearing on why they sought medical care.
Dretler also sees patients with multiple concurrent infections. “People who have very low white blood cell counts from chemotherapy might be admitted because of bacterial pneumonia or foot gangrene. They may also have covid, but covid is not the main reason why they’re so sick.”
If these patients die, covid might get added to their death certificate along with the other diagnoses. But the coronavirus was not the primary contributor to their death and often played no role at all.
Death Registration
Browse the articles related to this topic below.
Join our community on Guilded.
More than 650,000 deaths were registered in the UK in 2022 – 9% more than 2019.
This represents one of the largest excess death levels outside the pandemic in 50 years.
Though far below peak pandemic levels, it has prompted questions about why more people are still dying than normal.
Data indicates pandemic effects on health and NHS pressures are among the leading explanations.
https://web.archive.org/web/20230110142505/https://www.bbc.co.uk/news/health-64209221
UK health and statistics authorities allegedly used 14 inconsistent ways to define fatalities.
Many who died early in the pandemic were never actually tested for the virus while others may have died from something else entirely, according to experts.
…The Oxford study, from 800 freedom of information requests, found some deaths were attributed to Covid just because a care home provider said so and coronavirus was rife.
The report stated: “At the beginning of the pandemic, Public Health England linked data on positive cases to the NHS central register of patients who died.
“This definition meant that a patient who tested positive would be counted as a Covid death even if they were run over by a bus several months later.”
Did official figures overestimate Britain’s grim Covid death toll?
It’s a question that has been asked persistently by medics and members of the public alike almost since the start of the pandemic.
…Last week, in the first of a series of special reports probing the science that has underpinned our pandemic response, The Mail on Sunday set about tackling the ongoing concerns that tests used to diagnose Covid were picking up people who were not actually infected.
The conclusion of some scientists was, yes, they did. And there were those who maintained that despite shortcomings, PCR swabs – used by millions – were accurate enough.
Daily reported Covid death figures are too high because people are dying from conditions unrelated to the virus after testing positive, Sajid Javid has admitted.
On Wednesday, there were 359 deaths reported in Britain, but the Health Secretary said that “many” people were being included in the count who “would not have necessarily died of Covid”.
His comments came after death data from the Office for National Statistics (ONS) show a large discrepancy in weekly death registrations compared to the figures released on the Government dashboard.
For the week ending Jan 7, the UK Health Security Agency reported 1,282 deaths of people who had died within 28 days of testing positive for coronavirus.
However, ONS data show there were just 992 death registrations with Covid mentioned on the death certificate in that week.
An Office for National Statistics FOI request revealed 6,183 deaths recorded where COVID-19 was the only cause mentioned on the death certificate, between 1 February 2020 to 31 December 2021.
You asked
Please supply deaths caused solely by covid 19, where covid is the only cause of death listed on the death certificate, broken down by age group and gender between feb 2020 up to and including dec 2021.
Please supply the number of autopsies carried out on those where covid was the only cause stated.
We said
Thank you for your enquiry.
We have provided analysis on COVID-19 as the only cause of death by age and sex in England and Wales for your requested time period.
| Age group | Males | Females |
|---|---|---|
| <1 | 1 | 0 |
| 1-4 | 0 | 0 |
| 5-9 | 0 | 0 |
| 10-14 | 0 | 1 |
| 15-19 | 1 | 0 |
| 20-24 | 4 | 1 |
| 25-29 | 12 | 3 |
| 30-34 | 24 | 7 |
| 35-39 | 42 | 15 |
| 40-44 | 52 | 24 |
| 45-49 | 87 | 43 |
| 50-54 | 138 | 52 |
| 55-59 | 234 | 92 |
| 60-64 | 254 | 102 |
| 65-69 | 279 | 119 |
| 70-74 | 357 | 204 |
| 75-79 | 395 | 252 |
| 80-84 | 492 | 402 |
| 85-89 | 470 | 533 |
| 90+ | 520 | 971 |
EXCLUSIVE: UKHSA data shows infections are dropping in 96% of the country’s nearly 7,000 neighbourhoods
Parts of Castle Point, Shropshire and Bexley have seen infections fall by more than 70% week-on-week
And MailOnline analysis shows Omicron wave deaths were seven times lower than the peak last winter
Official figures show half as many Covid patients were in hospital at one time compared to the Alpha peak
And 4.5 times fewer patients were moved to critical care beds during the latest wave compared to last winter
Coronavirus cases are now falling in virtually every area of England, official figures show as the Omicron wave continues to collapse with deaths six times lower than in the second wave.
Some 6,519 out of 6,790 neighbourhoods (96 per cent) around the country recorded a fall in infections in the week to January 11, according to the UK Health Security Agency (UKHSA).
You asked
Please can you advise on deaths purely from covid with no other underlying causes.
We said
Thank you for your request.…Please see below for death registrations for 2020 and 2021 (provisional) that were due to COVID-19 and were recorded without any pre-existing conditions, England and Wales.
2020: 9400 (0-64: 1549 / 65 and over: 7851)
2021 Q1: 6483 (0-64: 1560/ 65 and over: 4923)
2021 Q2: 346 (0-64: 153/ 65 and over: 193)
2021 Q3: 1142 (0-64: 512/ 65 and over: 630)
Christopher Chope MP raises the figures for damage caused by Covid-19 vaccines in Parliament: “There’s a lot more damage being done to our citizens as a result of Covid-19 vaccinations than in any other vaccination program in history.”
Backup mirrors:
Excess deaths have not been this high since the week ending Feb 19, when 2,182 extra deaths were registered – 18.8 per cent above the pre-2020 five-year average.
Although some of the increase in excess deaths can be explained by the recent rise in deaths involving Covid, most were not linked to the virus.
Kevin McConway, emeritus professor of applied statistics at The Open University, said: “These excess deaths can’t all be explained by deaths of people who had Covid-19. In the most recent week, for England and Wales there were 1,270 more deaths than the five-year average – that’s 14 per cent higher than that average.
…Deaths in private homes have been well above the 2015-19 average almost every week since April last year. Before Covid, around a quarter of deaths occurred at home but that has since risen to one third, according to research by the King’s Fund.
Funeral firm Dignity said profits have fallen amid a marked drop in UK deaths since April as the group’s new boss outlined his turnaround plans.
The group said that following a 27% surge in first quarter deaths to 204,000 during a Covid-hit start to the year, the number of deaths fell below the five-year average in April and May and were 7% lower.
This has left underlying operating profits “slightly” lower year-on-year at £30.7 million for the 21 weeks to May 21, according to Dignity.
The number of people dying with flu and pneumonia on their death certificate in England and Wales is now 10 times higher than those with Covid, figures show.
The latest weekly data on deaths from the Office for National Statistics (ONS) show that there were 84 deaths mentioning Covid in the week ending June 11. There were 1,163 involving flu and pneumonia.
Registered Covid deaths fell by 14 per cent since the last update, in the week ending June 4, when 98 deaths were recorded.
Covid deaths now make up just 0.8 per cent of all deaths – down from 1.3 per cent in the previous week, despite the fact that week included the late May bank holiday, meaning there were fewer death registrations.
…The figures are much lower than would usually be expected for respiratory disease at this time of year. The five-year average for deaths involving flu and pneumonia in the same week is 1,704.
https://www.telegraph.co.uk/news/2021/06/22/flu-pneumonia-deaths-now-ten-times-higher-covid/
Nearly 40 per cent of recently registered Covid deaths in England and Wales were people who died primarily from another condition, latest figures from the Office for National Statistics (ONS) show.
Out of 107 Covid deaths registered in the week ending May 21, just 66 had coronavirus recorded as the underlying cause of death, 61.7 per cent.
Britain recorded no new deaths within 28 days of a positive COVID-19 test on Tuesday.
The last time Britain recorded no deaths was in March 2020, before the country had entered its first lockdown. The figure on Tuesday relates to how many deaths have been reported and it comes after a national holiday on Monday – a factor which has in the past skewed the data.
…Britain’s overall death toll from the pandemic stands at 127,782 and is the fifth highest in the world, according to Johns Hopkins University data.
https://www.reuters.com/world/uk/uk-reports-no-new-covid-19-deaths-3165-new-infections-2021-06-01/
This is not because Ted Mooney contracted coronavirus in the very good (and expensive, it must be said) care home three miles from our house, as statistics will now state.
Because he did not. Yet the principal cause of death is set down officially as Covid-19 — and that, in my view, is a bizarre and unacceptable untruth.
…They agreed that, yes, it must distort the national figures — ‘and yet the strangest thing is that every winter we record countless deaths from flu, and this winter there have been none. Not one!’
The truth is that there was never a question of whether this Government would impose another lockdown on the UK in 2021. Lockdown isn’t a consequence of the failure of coronavirus-justified programmes and regulations: it’s the product of their success in implementing the UK biosecurity state. After a brief summer recess under the system of tiered restrictions, the following winter will see the lockdown of the UK imposed again under newly notifiable diseases from new viruses and new strains, new protocols for certification and new criteria for deaths, the new medical categorisation of new cases which, like the present ones, present little or no threat to public health, but which like it will be used to enforce new technologies, new programmes and new regulations. This is the ‘New Normal’ we were promised, and it’s being built on a foundation of lies, damned lies and statistics.
Grampian NHS Board via a Freedom of Information (FOI) request. Number of deaths between February and November 2020 where COVID-19 was the sole cause:
- 15 confirmed
- 5 suspected

In the UK, a Covid death is recorded if a person has died within 28 days of the first positive test.
However, what the figures do not tell us is to what extent the virus is causing the death.
In some cases, it could be a major cause. In others, it could simply be a contributory factor or perhaps just present in a person’s system when they have died of something else entirely.
Theoretically, a 90-year-old cancer patient already on palliative care could die but have coronavirus in their system at the time of death. That could be recorded as a coronavirus death.
Number of deaths, crude and age-standardised mortality rates from 1938 to 2020. Age-standardised mortality rates start in 1942.
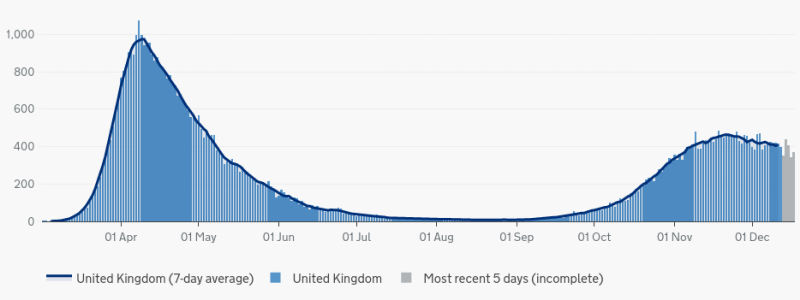
Deaths within 28 days of positive test by date of death last updated on Sunday 20 December 2020.