Nature published a comprehensive study this week on cardiovascular risk including a total of over 11 million patients that has made a few headlines. The aim was to identify the cause of increased cardiac pathology. It should have been a very simple study comparing four groups:
Not infected and never vaccinated
Not infected and vaccinated
Infected but not vaccinated
Infected and vaccinatedIt is hard to believe the authors did not look at these groups, but whatever was found when comparing them remains a mystery.
Instead, the following groups were compared:
Not infected and never vaccinated data from 2017
Not infected, including vaccinated and not vaccinated
Infected but not vaccinated
Infected with vaccinated people included but using modelled adjustmentsWhen studies with huge datasets use modelling and fail to share data prior to their adjustments alarm bells should start ringing. Therefore, I took a deeper dive to see what else was questionable.
Lockdown Sceptics
Browse the articles related to this topic below.
Join our community on Guilded.
Contrary to the claims made by Dr Rachel Clarke and Professor Stephen Powis last month and used to blame the unvaccinated for the mounting troubles of the NHS, new data out this week shows that the majority of Covid ICU admissions in October and November were among the vaccinated, not the unvaccinated.
The latest report from ICNARC shows that of Covid ICU patients in England, Wales and Northern Ireland, 50.5% in October and 50.7% in November were double vaccinated. Add to that the 2.8% in October and 1.8% in November who were single-vaccinated and you get overall vaccinated proportions of 53.3% in October and 52.5% in November. That compares to 46.7% unvaccinated in October and 47.5% in November. Note that the unvaccinated here includes people who received a vaccine less than 14 days prior to the positive Covid test, so includes some (an unknown number) who are actually single vaccinated.
Health at a Glance 2021 – OECD
Health at a Glance provides a comprehensive set of indicators on population health and health system performance across OECD members and key emerging economies. These cover health status, risk factors for health, access to and quality of health care, and health resources. Analysis draws from the latest comparable official national statistics and other sources.
Alongside indicator-by-indicator analysis, an overview chapter summarises the comparative performance of countries and major trends. This edition also has a special focus on the health impact of COVID-19 in OECD countries, including deaths and illness caused by the virus, adverse effects on access and quality of care, and the growing burden of mental ill-health.
https://www.oecd-ilibrary.org/social-issues-migration-health/health-at-a-glance_19991312
Commentary by The Daily Sceptic:
UK Life Expectancy in 2020 Was Still at 2010 Levels and Over 80, OECD Report Shows – The Daily Sceptic
Despite all the daily reports of deaths, the running total of over 165,000 Covid deaths, and the repeated lockdowns imposed to protect a health service ever on the brink of collapse, the country has experienced a mortality rate no worse than 2009. I don’t know about you, but I can remember 2009. I don’t recall any lockdowns and panicking, or coerced experimental medicine, or bodies piling up in the morgues. Yet it was a worse year for deaths than the great pandemic year of 2020. Let that sink in.
…The OECD analysis is in line with the analysis done in April by economist John Appleby writing in the BMJ. The chart below shows that age-standardised mortality in 2020 was lower than in 2008 and every year prior to it.
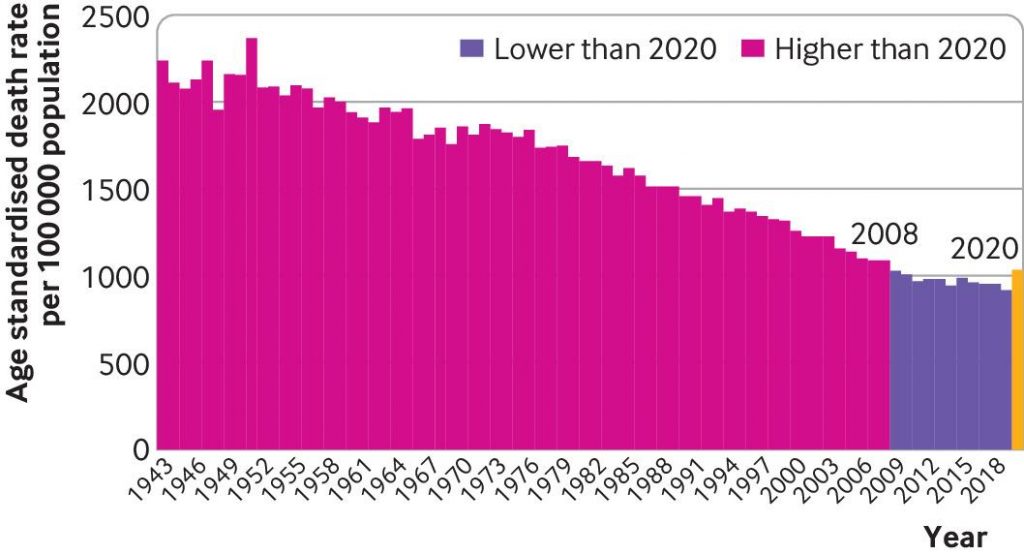
There have been at least seven peer-reviewed studies which look at the question of lockdowns from a data point of view, and all of them come to the same basic conclusion: lockdowns do not have a statistically significant relationship with Covid cases or deaths. Here is a list of them with a key quote for ease of reference.
- “Comparing weekly mortality in 24 European countries, the findings in this paper suggest that more severe lockdown policies have not been associated with lower mortality. In other words, the lockdowns have not worked as intended.” “Did Lockdown Work? An Economist’s Cross-Country Comparison” by Christian Bjørnskov. CESifo Economic Studies March 29th, 2021.
- “Stringency of the measures settled to fight pandemia, including lockdown, did not appear to be linked with death rate.” “Covid-19 Mortality: A Matter of Vulnerability Among Nations Facing Limited Margins of Adaptation” by Quentin De Larochelambert, Andy Marc, Juliana Antero, Eric Le Bourg, and Jean-François Toussaint. Frontiers in Public Health, November 19th, 2020.
- “Lockdowns do not reduce COVID-19 deaths.” “Government mandated lockdowns do not reduce Covid-19 deaths: implications for evaluating the stringent New Zealand response” by John Gibson. New Zealand Economic Papers, August 25th, 2020.
- “While small benefits cannot be excluded, we do not find significant benefits on case growth of more restrictive NPIs.” “Assessing Mandatory Stay‐at‐Home and Business Closure Effects on the Spread of COVID‐19” by Eran Bendavid, Christopher Oh, Jay Bhattacharya, John P.A. Ioannidis. European Journal of Clinical Investigation, January 5th, 2021.
- “Previous studies have claimed that shelter-in-place orders saved thousands of lives, but we reassess these analyses and show that they are not reliable. We find that shelter-in-place orders had no detectable health benefits, only modest effects on behaviour, and small but adverse effects on the economy.” “Evaluating the effects of shelter-in-place policies during the COVID-19 pandemic” by Christopher R. Berry, Anthony Fowler, Tamara Glazer, Samantha Handel-Meyer, and Alec MacMillen, Proceedings of the National Academy of Science of the USA, April 13th, 2021.
- “We were not able to explain the variation of deaths per million in different regions in the world by social isolation, herein analysed as differences in staying at home, compared to baseline. In the restrictive and global comparisons, only 3% and 1.6% of the comparisons were significantly different, respectively.” “Stay-at-home policy is a case of exception fallacy: an internet-based ecological study,” by R. F. Savaris, G. Pumi, J. Dalzochio & R. Kunst. Scientific Reports (Nature), March 5th, 2021.
- “Full lockdowns and wide-spread COVID-19 testing were not associated with reductions in the number of critical cases or overall mortality.” “A country level analysis measuring the impact of government actions, country preparedness and socioeconomic factors on COVID-19 mortality and related health outcomes” by Rabail Chaudhry, George Dranitsaris, Talha Mubashir, Justyna Bartoszko, Sheila Riazi. EClinicalMedicine (The Lancet) 25 (2020) 100464, July 21st, 2020.
Briefing paper for MPs authored by:
- Clare Craig BM BCh FRCPath
- Jonathan Engler MBChB LLB
- Mike Yeadon BSc Hons (Biochem-tox) PhD (Pharmacol)
- Christian McNeill LL.B and Dip LP
Stop mass-testing using PCR in the UK and replace with Lateral Flow Tests where required. If we are correct, this single measure alone will cause a sudden drop in “cases” (as seen in Liverpool) and allow the UK to return to normal life within weeks.
Other recommendations as detailed later in this document. It should be noted that legal cases and technical challenges to PC
https://lockdownsceptics.org/wp-content/uploads/2020/11/MP-briefing-26-Nov-2020.pdf
Code Review of Ferguson’s Model
All papers based on this code should be retracted immediately. Imperial’s modelling efforts should be reset with a new team that isn’t under Professor Ferguson, and which has a commitment to replicable results with published code from day one.
On a personal level, I’d go further and suggest that all academic epidemiology be defunded. This sort of work is best done by the insurance sector. Insurers employ modellers and data scientists, but also employ managers whose job is to decide whether a model is accurate enough for real world usage and professional software engineers to ensure model software is properly tested, understandable and so on. Academic efforts don’t have these people, and the results speak for themselves.